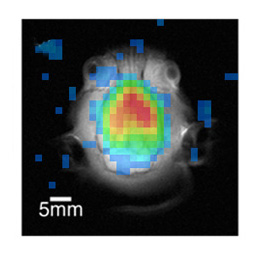
 Superposition of a false color 129Xe image onto a 1H spin-echo image showing that the 129Xe signal arises entirely from within the brain as well as reduced 129Xe in the cerebellum. Image from http://bearhat.rad.med.umich.edu/˜scott/xeimages.cfm |
Researchers at several institutions around the US reported-progress toward developing next-generation magnetic resonance imaging (MRI) technology, to image the respiratory system during the APS Centennial meeting . Minimally-invasive, high-resolution imaging is expected to have critical clinical and research applications, including surgical pre-screening, assessing disease progression and response to therapy, investigating fundamental lung physiology, and studying the pulmonary effects of harmful agents.
According to Ron Walsworth of the Harvard-Smithsonian Center for Astrophysics (HSCA), the respiratory system has been the most challenging for non-invasive medical imaging. The current clinical methods involve nuclear-based techniques such as computed x-ray tomography of inhaled radioactive isotopes, which provide mediocre image resolution and involve significant exposure to ionizing radiation. Current MRI scanners produce high-resolution images using a powerful magnetic field to polarize protons in water molecules in the patient's body, much as a bar magnet aligns iron filings. These polarized protons are detected by radio waves and are processed in a computer to produce detailed images of internal soft tissue.
However, the lung has a convoluted tissue-gas interface-crucial for effective gas exchange between the blood and air-and low concentrations of water making conventional MRI ineffective. The new MRI machines under development detect signals from laser-polarized molecules of xenon and helium-3, producing images of lungs and airways with excellent anatomical detail in both animals and humans. It has also been used to image the lungs of patients with Chronic Obstructive Pulmonary Disease (a class of diseases which includes emphysema), with clear indications of regions of low lung ventilation caused by the disease, and much higher resolution than any other imaging technique.
The HSCA team recently demonstrated laser-polarized noble gas MRI using a simple, low-cost MRI system that provides a magnetic field about 1,000 times smaller than conventional MRI machines. Advantages include the possibility of using open geometry magnets — instead of the "claustrophobia-inducing closed magnets used in many hospital MRI units," says Walsworth — as well as low-cost portable MRI instruments for imaging lungs and sinuses. Furthermore, using gases and low magnetic fields will aid in such non-medical applications as imaging porous materials and the interior of metallic objects.
A group of researchers at the University of Michigan are investigating MRI using a similar customized laser optical pumping system to polarize molecules of xenon gas, delivered via single-breath doses. According to Scott Swanson, U-M Medical School, xenon has several advantages. "The gas dissolves in the bloodstream is non-reactive and safe in measured doses, and can be polarized in higher concentrations than water molecules. It also differentiates between tissue, blood, and gas.
Timothy Chupp, a U-M professor, says "While many technical obstacles remain before the technology is ready for human use, our results indicate it could be used to monitor perfusion through the heart, lungs and kidneys." Future research will focus on finding ways to increase xenon polarization to 5% to 35%, which will provide the resolution required for clinical applications.
Perhaps the best indication of the technology's potential is the emergence of a commercial company, Magnetic Imaging Technology, Inc. (MITI) in Durham, NC, founded to develop the advanced tools and capabilities needed to make hyperpolarized gas MRI imaging commercially feasible.
©1995 - 2024, AMERICAN PHYSICAL SOCIETY
APS encourages the redistribution of the materials included in this newspaper provided that attribution to the source is noted and the materials are not truncated or changed.
Editor: Barrett H. Ripin
Associate Editor: Jennifer Ouellette
July 1999 (Volume 8, Number 7)
Articles in this Issue

